This article looks at burnout from a personal perspective and follows on from Mark Turner’s article in the July 2020 edition of Companion. Unlike other articles I have read on this topic which tend to be fairly high-level overviews, this is different in that it describes, and is based on, personal experience.
Burnout is a frequently misused and misunderstood term, often used as a buzzword to get the attention of the reader. This short-changes those who have been unfortunate enough to experience burnout themselves; it can have life changing consequences to those it affects and has a large and unquantifiable cost to businesses.
Introduction
Burnout is currently sitting at an uncomfortable junction between being the syndrome “everyone” is collectively suffering from, maybe even a status symbol equated to overwork and dedication to the job, and a mental illness with a heavy stigma attached.
It is neither.
We need to truly understand what burnout is, and what it is not, in order to prevent more people from succumbing to the considerable suffering and health issues that burnout causes and, more importantly, to recognise it in yourself. Burnout is more than just being tired and stressed, which unfortunately seems to have become normal for humans in the 21st century as the lines between work and home life have become increasingly blurred.
Burnout research is growing but is still in its early stages and most so far have been small-scale occupational studies leading to non-validated tools for assessment and a varied quality of research. We don’t know the true extent of burnout in the profession or the wider population, but one study suggested one in seven young vets will experience burnout within 10 years of graduating.

What is burnout?
Burnout is the end result of the body’s response to long-term high-level stress. The body’s stress reaction is a useful protective response to potential danger, but it is not supposed to be activated long-term. The saber-toothed tiger would go away and we’d return to the safety of our cave and family. But now the tiger is in our cave, in the form of smart phones, emails, messages, and when not in the safety of the cave we are constantly on the run from the tigers of work pressures and life busyness. Due to chronic stress, we are gradually depleted over time, so we don’t notice the subtle changes that burnout brings until they are dire or are so visible from the outside that someone else notices. Burnout covers a spectrum of degrees from chronic, perpetual tiredness and mild apathy to life, to fulminant burnout where your body suddenly puts on the brakes and you can’t get out of bed, or something in your body breaks.
Physically our bodies go through changes when we are burning out. It affects the structure (which can be seen on MRI) and function of the brain and, in particular, the neuro-endocrine axis affecting memory, emotional regulation and attention. The effects are similar to those seen in severe early-life trauma victims. Outside the brain there are massive changes in the body which have serious physical consequences: hypertension, type 2 diabetes, coronary heart disease, musculoskeletal pain, prolonged fatigue, headaches, gastrointestinal issues, respiratory problems, a higher risk of severe injuries and increased mortality. Psychological effects include insomnia and depressive symptoms.
The consequences of burnout are complete mental, emotional, and physical exhaustion accompanied by depersonalisation or cynicism (an attempt to put more distance between oneself and the source of the stress) and lowered ability in almost every aspect of daily life. Freudenberg, one of the original researchers into burnout, describes 12 stages of burnout which, although it’s unlikely that someone would go through them all in turn, is a useful reference for describing the emotions and behaviours that lead to full-on burnout.
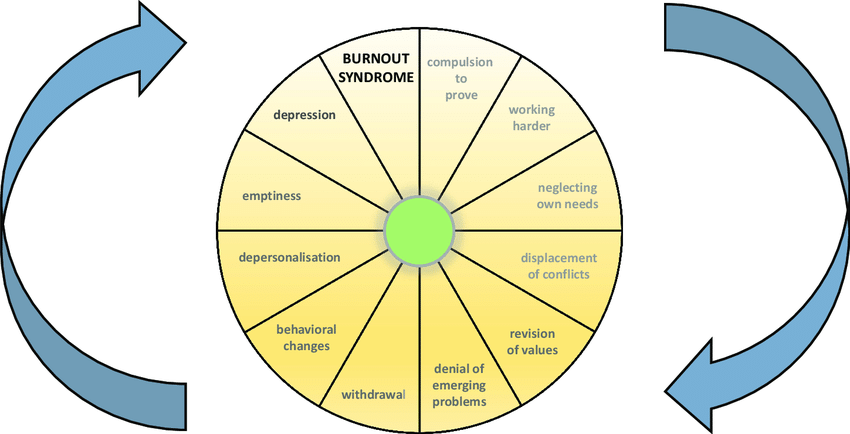
What is it not
Now we have more of a handle on what burnout is, let us address what burnout is not.
- It is not just stress. It is not perception of stress. It is not a state of mind.
- It is not depression or compassion fatigue or moral injury. Burnout is considered by some researchers to be a precursor or risk factor for depressive illness. One stage of burnout shares common features with depression (indifference, helplessness, exhaustion, apathy and believing the future holds nothing for the sufferer) but burnout is compounded by the work environment and, as with other environmentally-induced illnesses, will get better with time from just being removed from that environment. In contrast, depression is more general and context-free. It is crucial to understand this as those with burnout may be falsely labelled as having depression and/or anxiety disorders, leading to inappropriate treatments.
- It is not personal weakness, a failure to cope or a lack of resilience. In fact, it is often just the opposite; it is because you are strong enough to push through the many warning signs your body is trying to give you, overusing your strengths, that you have reached this extreme.
- It is not a synonym for exhaustion. Yes, exhaustion is a large part of what you feel in burnout but it is not the sole aspect.
- It is not a disease, a medical condition or mental illness.
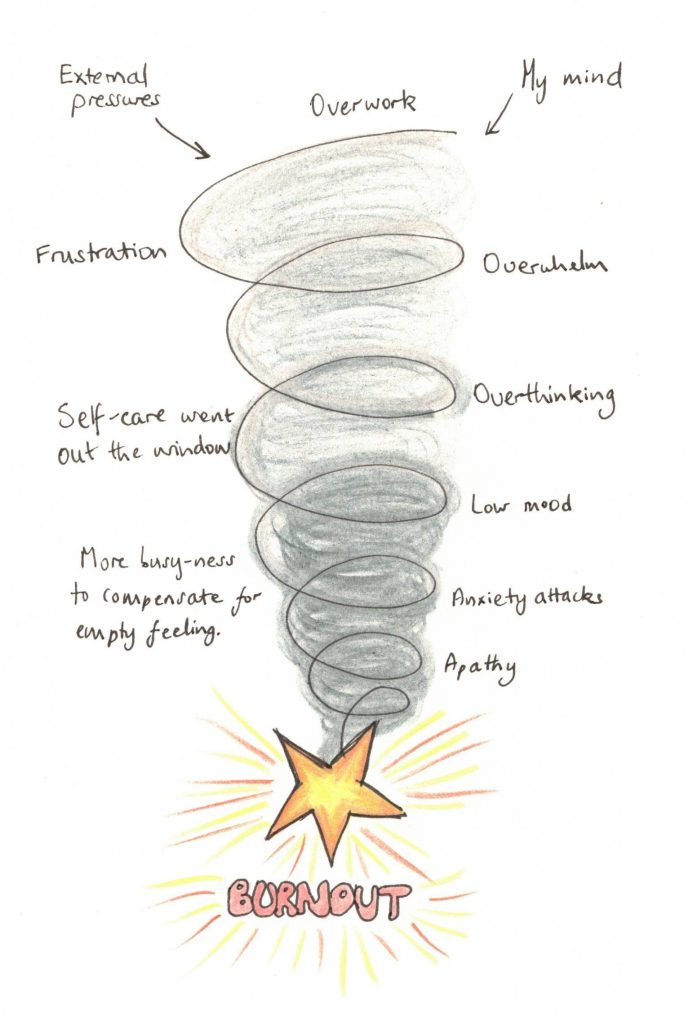
What causes it
Burnout is caused by chronic stress to which many factors contribute, both intrinsic and extrinsic. You can be doing the same work as someone else and burnout while they don’t, but it is not personal weakness that leads to this difference. The chronic stress comes from an imbalance of job resources and demands but how we experience and deal with the stress is personal. It is about the overall experience of work, not the number of work hours.
Intrinsic factors lead to inner pressures, especially personality factors, that alter how individuals evaluate their personal stressors plus the sense of insufficient reward for the work. Those particularly susceptible include high achievers and those with perfectionist tendencies, those with a need for external recognition or who focus on pleasing other people and putting others’ needs first, and those for whom work is a large part of their identity. Women are also at higher risk of burnout as they place a greater emphasis on caring responsibilities which adds to mental load. Does this not sound familiar for a good proportion of veterinary professionals?
Extrinsic factors that contribute to burnout are those that lead to unsustainable workloads and, more importantly, work that is incongruent with personal or organisational values, both of which are common in the veterinary industry. These include high demands and time pressures, ongoing chaotic scheduling, problems with leadership and collaborative work, contradictory values, poor working atmosphere, lack of freedom or control in how work is accomplished, and the lack of influence over many of these aspects. The type of work needs to be considered and whether it is meaningful to the worker – ‘helping animals’ is not enough, especially when veterinary work is mainly helping people. The imbalance between skills and demands is a strong determinant for burnout, especially for those at the start of their career or for those that take on new responsibilities without training and support such as a promotion to a manager level or starting their own business.
What does it feel like personally?
This section is difficult for me to write, even 18 months after I suffered fulminant burnout. It brings up painful emotions and also fills me with guilt for not being able to cope, but until we can openly discuss topics relating to mental health and understand how they happen, we have little chance to stop others from suffering the same.
I was well on the way to burnout when COVID occurred, but I had no insight into what was happening to me or how to fix it; all I knew was that I had to keep going and believe it would all be fine at some point. I was stuck trying to keep an income coming in and trying to find a meaningful career. I kept busy to distract from self-doubts as to whether I was any good, triggered by years of additional training, qualifications and experience being under-recognised by managers. I started having anxiety attacks at work and my anxiety totally spiralled out of control leaving me to hide in the toilet as the only place to get away from people, especially an unsympathetic boss who felt that employees lacked “resilience training”, while I cried or hyperventilated. I felt extreme fatigue all the time and would fall asleep in any situation, yet restful sleep at night eluded me as I often woke for hours and stressed over the on-call phone or a case that could have gone better. I procrastinated and struggled to focus on tasks, and my usually good memory disappeared as I struggled through a massive work project. Self-care felt like just another task that I had no energy for. I felt lost and was just going through the motions of life, not living, just surviving in limbo awaiting the time when it would get better. I felt detached, like all this was happening to someone on TV because the whole situation was out of my control. Compounded by a toxic work environment and being pressured to betray my own values, I was burning out fast.
When my fulminant burnout struck, I just couldn’t summon the energy to do anything. I slept, then slept some more. I would read a book or watch something on TV but it would just wash over me and my brain felt like mush. Nothing felt enjoyable, there was no emotion, I was just numb. I took 4 months off work and gradually during that time, my old self came back again and I found joy in what I was doing. I came to realise that it wasn’t that I was too weak to hack it, that I did still enjoy being a vet, and it was the work environment that needed to change.

What does it look like to others?
Once signs of burnout are visible to others, the person is already deep in burnout. Here are some things to keep in mind if someone doesn’t act as you have come to expect them to.
- The person is no longer joyful or having fun.
- They may look vacant and not respond normally.
- They have no energy, perhaps they fall asleep at lunch.
- They are worse at controlling or suppressing negative emotions, become defensive or aggressive easily, or intolerant of changes.
- Working above and beyond – always the one to stay late, come in when extra shifts need covering, taking work home. They no longer do activities out of work if you ask what they did in their evening or weekend.
- Beyond that stage, they may then not care in situations when they used to, perhaps ‘quiet quitting’.
- The person stops taking care of themselves, such as not having their hair cut or washing as frequently.
- Someone who was once interested and participated in practice meetings and events no longer attends or shows a lack of interest.
Why is it so bad? We are all exhausted!
We all feel exhausted after a few difficult years in the profession and life in general, so what makes burnout so dangerous? For the individual, full burnout is quite frankly devastating and causes massive emotional distress and damage. The knock-on effects for physical and mental health and the health of the relationships around them is substantial. The recovery from burnout requires a not insignificant amount of time off work which can have repercussions for the person, even cost them their job. I have no doubt that the effects and the trauma felt by burnout victims contribute to the retainment issues the profession is currently having.
For the profession and workplaces, people that are burning out have reduced productivity and become disengaged from the job, reducing efficiency, increasing errors, and leading to retention issues. Burnout reduces creativity, problem solving and acceptance of change, just when these aspects are even more important for businesses trying to adjust to the changing environment. Burnout can affect everyone, employees and bosses, and it often affects the best employees, the ones that give their all and more to the job. A recent paper on the economic impact of burnout on the US vet industry, estimated $1-2 billion annually of lost revenue.
Prevention
One person succumbing to burnout in a workplace is just the tip of the iceberg – there will be many more people below the water line that are in varying degrees of burnout. Employers need to recognise the crucial part the workplace has in contributing to burnout and that any solutions looking at the individual level alone are incomplete. Systemic changes in workplaces are needed when burnout occurs to any degree, in any individual. Sending staff on a resilience course and putting on yoga sessions are not the solutions to a team burning out, they just allow people to walk a few steps closer to the danger before the inevitable happens. Please seek specialist external help for organisational solutions on preventing burnout.
We also need to learn to recognise it in ourselves and stop before we get to fulminant burnout and learn to ask to help. Our brain is crap at telling us when we are doing too much – aching legs from a long run are an obvious reminder that you need to rest, but your brain can just power on through. Introspection and self-analysis are important in assessing ourselves, but they are not innate or even common abilities and need both training and courage. Talking to a therapist or a coach can help with outside perspectives, as well as skills such as stress management, changing the source of satisfaction from external to internal sources, and rethinking perfectionist tendencies and crystallising your values. Boundaries may also be a buzzword of the century, but they are essential for making sure we give ourselves enough time and importance to rest and recuperation, time with other people and other interests outside of the profession.
Treatment
If you are currently suffering from burnout, please know you will get better, there is light at the end of the tunnel and you will find joy again. Recovery needs two things: time (1-3 years for most people) and agency (control over your environment). For most people this means they can’t keep their recovery on track while remaining in the same work or even the same place of work, partly due to trauma associated effects, and so need to leave their job or even stop working entirely. I needed a 4-month complete break during which I didn’t do anything veterinary and reconnected with my interests, then 6 months staged return to clinical work. For me to control my workload and not compromise my values, I’ve found I need to work for myself and so I’ve set up a business.
As burnout sufferers, we are often told that we are the problem and therefore we need to find the solution, but this is not the way to treat or prevent burnout. Unfortunately, at this time there is little research or structured support for those undergoing burnout or trying to recover from it. I hope that with time, this will change.
Summary
Burnout is sometimes equated with exhaustion – it is far more than that – but no-one should be continually so exhausted that it affects the living of their life. Burnout is still seen as a rite of passage or badge of honour for some in the profession such as interns and residents, and those that fall by the wayside are derided as not being made of the right stuff – this must change for the health of everyone. If the potential ruin of a human life is not enough to be a wakeup call, perhaps the economic cost will.
This article was commissioned by and originally published in BSAVA Companion December 2022 issue which you can access here.

Leave a Reply